https://triblive.com/local/regional/regions-health-experts-alarmed-by-unacceptable-rise-in-maternal-deaths/
Western Pa. health experts alarmed by ‘unacceptable’ rise in maternal deaths
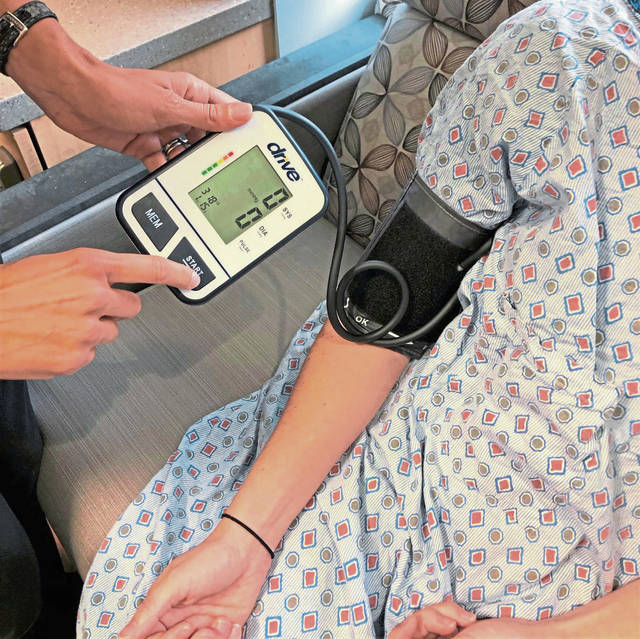
Local doctors say the rising number of maternal deaths in the state is “unacceptable” and “scary,” and they are working to create more comprehensive ways to care for pregnant and postpartum women.
According to data from the state Department of Health, an increasing trend in pregnancy-related deaths occurred from 2012-16 with 11.4 deaths per 100,000 live births.
For black women, that rate is more than double at 27.2 pregnancy-related deaths per 100,000 live births.
In the past two years, a 38-year-old woman from Greensburg died just weeks after her son’s birth and a 35-year-old Pittsburgh woman died during childbirth.
According to the World Health Organization, the United States has the highest maternal mortality rate in the developed world.
“It’s not just unacceptable,” said Dr. Marcia E. Klein-Patel, an obstetrician-gynecologist with Allegheny Health Network. “It’s, frankly, horrifying.”
Hospitals are doing everything from more training on being prepared for an emergency to monitoring patients more closely for issues that may arise postpartum.
According to the CDC, the cause of death for pregnancy-related deaths include hemorrhage, infection or sepsis, amniotic fluid embolism, thrombotic pulmonary or other embolism, hypertensive disorders of pregnancy, anesthesia complications, accidents related to the brain, cardiovascular conditions and other non-cardiovascular medical conditions.
While things like obesity, drug abuse, hypertension and age can be risk factors for illness or death, sometimes there are no indicators a woman might experience complications.
Being prepared
Klein-Patel said AHN does routine training so employees are knowledgeable on the correct process for addressing complications like a hemorrhage, which is one of the leading causes of death for women during and after delivery. Doctors make sure they have “hemorrhage carts” placed in key areas so they quickly have access to the right treatment.
Klein-Patel said it’s not just about making sure they are ready for what may happen in the hospital, but making sure women have what they need at any time — even before becoming pregnant.
She said making sure they are providing care for women that can help address other needs they may have such as housing, transportation or finding a job is an important piece to the puzzle.
“(We’re) trying to build in a case management service that can help all women when they have any issues that we can help with, then guide them to the resources in our community,” Klein-Patel said.
Access to care can be one of the risk factors that contribute to complications during and after delivery. So hospitals are making sure they are reaching out to patients in any way they can. Some patients who live in rural areas or don’t have easy access to transportation will go without care.
“As other community hospitals have closed their labor and delivery units, we’re trying to make sure we can see those patients in a timely fashion,” said Dr. Randi Turkewitz, an obstetrician-gynecologist with Excela Health in Westmoreland County.
Turkewitz said the health system also partners with other agencies such as Adagio Health, which helps provide access to care for uninsured and underinsured residents. She said trying to break the stigma for women who need these services is one of the challenges.
“I think a lot of people assume that they’re going to be judged,” she said. “We’re here for them.”
Meeting patients where they are
UPMC started using its telemedicine program, in which doctors can interact with patients via video or phone, to reach out to postpartum women who need their blood pressure monitored. They piloted a program last year with nearly 500 women who had preeclampsia, eclampsia or hypertension.
“What we were hoping to do with this program is to reduce some of those barriers to care in that period,” said Dr. Alisse Hauspurg, assistant professor of obstetrics, gynecology and reproductive sciences at University of Pittsburgh.
Women can check their own blood pressure at home and then report the numbers to a nurse who checks for anything that would raise a red flag.
“We can tell that we are more frequently changing medicine, starting women on medication who otherwise might not have been on treatment during this period,” Hauspurg said of the program.
Dr. Hyagriv Simhan, executive vice chair of obstetrical services at UPMC, said hypertension is not only one of the leading causes of maternal death and illness, but it often can have lifelong effects such as an increased risk in heart attack and stroke.
“The benefits, we think, go beyond just these six weeks after (delivery),” he said.
Addressing racial disparity
Amanda Shafton, lead midwife with Allegheny Health Network, is also studying “implicit bias,” which is the unconscious attribution of particular qualities to a member of a certain social group, that doctors have when treating black patients that could lead to negative outcomes. The study is part of her doctoral work.
“We see things like less time interaction between provider and patients,” she said. “Patients say they’re less trusting of their providers.”
Shafton said she tries to educate doctors and nurses on how to recognize their own implicit bias so they can be aware it may be influencing the care they give.
“You go into (medicine) because you want to take good care of people — and you want to take good care of everybody,” she said. “We have to recognize that’s just not happening.”
Copyright ©2026— Trib Total Media, LLC (TribLIVE.com)
